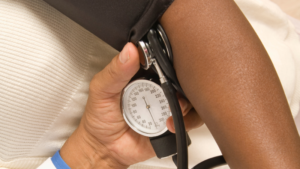
Approximately 20 percent, or $250 billion worth of Medicare, Medicaid or commercial/ office/ home health care could be possibly virtualized, according to McKinsey and Company findings.¹ And so, the future of digital health is looking bright. This rings particularly true for Remote Patient Monitoring (RPM) and its newest variations. As PHE flexibilities continue to be made permanent, clinicians can have hope that mobile health will cement its place as a substantial part of any care routine. Here’s what RPM trends clinicians can expect this year:
Mainstream Adoption
According to a recent survey, 40 percent of physician offices currently utilize RPM and 70 percent of those practices report increased improvements in patient engagement, satisfaction and revenue cycles, along with the opportunity to create more space for high-priority in-office visits.²
70 percent of practices surveyed reported increased improvements in patient engagement, satisfaction and revenue cycles.²
In the same survey 60 percent of c-suite executives and clinical leaders say that RPM is a critical opportunity for identifying gaps in care and believe it will become the new standard of care over the next two years.²
The industry’s mainstream adoption of RPM has only been accelerated by the COVID-19 pandemic. Many clinicians used the service to triage patients exhibiting signs of COVID-19. Consequently, these clinicians were able to glean insight on how to run an RPM program, if they had never before, as well as imagine other possibilities in which RPM could be possible for their patient population. Patients were able to see how easily home health could be integrated into their care routine and how it could help them maintain contact with their providers in case of any concerns.
The value of RPM extends beyond what practices are routinely in place. While collecting physiological data is a great benefit, RPM can also pinpoint long-term trends to help form guidelines around therapies, procedures and tests that elevate the quality of care and increase revenue.²
This could mean the ways in which clinicians use RPM could become more complex. Rather than just using the modality as a way to track and report, clinicians could also use the data to expose trends and build stories about their patient populations as a way to better understand them.
Beyond the Wrist Innovation
So far, clunky hardware has been the standard for RPM programs. However, many innovators are looking to miniaturize devices, so that they integrate seamlessly with a patient’s daily life, allowing continuous monitoring to barely be a thought.
Apple is one of the leaders in portable RPM innovation, with its widely recognized smartwatches and health apps. However, it should be noted that in order for CMS to reimburse clinicians for RPM, the device used must not only be useful for the diagnosis and treatment of the patient’s condition, but it must also be FDA-approved.³ Apple has bypassed FDA approval by advertising its products for the intended use of “general wellness.”⁴ Clinicians looking to be reimbursed, should be aware of their certified options.⁴
But many other companies are in the process of developing and seeking FDA approval for devices that go even further than smartwatch wear. For example, companies such as Siren and Owlet have developed wearable and machine washable smart socks that can monitor signs of inflammation, heart rate, oxygen level and sleep trends.⁴ Other innovators at the CES 2022 showcase for RPM, demonstrated the possibilities for devices such as armbands, rings and skin patches.⁴
LifeSignals recently received FDA approval for its single-use wearable biosensor that simultaneously monitors electrocardiography, heart rate, respiration rate, skin temperature and body posture data for up to five days.
For long-lasting and cost-effective devices of the future, some researchers are recommending Human Body Communication (HBC) technology. This involves ingested or implanted medical devices that use electrical signals to transmit data through connective tissues. This then allows for clinicians to take advantage of “in-, on-, and off-body communications.”
Equally on trend are non-invasive smart devices that continue to raise RPM’s usage. In Japan, Aevice Health raised $2.1M to bring its AI-powered wearable stethoscope to Japan for home monitoring use.⁵
These innovations signal a larger trend of increasing the usability and compatibility of RPM in a patient’s daily life. We may be a few years away from widespread commercial use for these products, but the growing influence can’t be ignored.
Increased Use in RPM for Specialty Providers
The variety in RPM inventions means that RPM can not only be tailored for use in specialty areas, but designed specifically for them. This inclusivity in innovation will lend itself to a whole new definition of “whole-body wellness.”
Currently, RPM use is mainly focused on hypertensive, diabetic and COVID-19 patients. While this covers a substantial amount of the nation’s patient population, vulnerable patients could need RPM intervention in multiple domains.
For example, in the U.S., the maternal death rate for black women is three times higher than it is for white women. To combat this saddening disparity, UnitedHealthcare launched a pilot maternal monitoring program in Tennessee. The goal will be to monitor metrics that specifically involve pregnancy risks. Hopefully payviders, like UnitedHealthcare, continue to lead the way for other public and private payers to make RPM a standard in every specialty.
Another specialty consistently and increasingly using RPM are researchers and providers focused on Alzheimer’s treatment. University of Pennsylvania school of medicine recently received $20M to launch an RPM program for Alzheimer’s patients, and monitor the effects of the intervention.⁶ Similarly, companies such as Apple, Merck and Biogen have begun launching experiments to see if mHealth technology can help identify signs of cognitive decline, including Alzheimer’s disease.⁶
And no worries for patients who need more private issues monitored as well. Researchers at Duke University developed an AI tool, installed inside of toilet pipes, with the purpose of monitoring chronic gastrointestinal issues, such as inflammatory bowel syndrome or irritable bowel syndrome. The tool photographs the stool as it passes through the pipes and sends the images to the physician. The physician can then analyze the stool to detect any abnormalities or presence of blood in the sample.⁷ Innovations such as these not only have important implications for the spread of RPM, but also its practicality. Seeing as this AI tool makes use of something every patient has in their homes–toilets– and requires minimal digital skill from patients, it eliminates many barriers facing the RPM industry today.
Rural providers are also increasingly using RPM for their at-risk populations in an effort to stay connected. The distance between the office and a patient’s home is often longer than what’s ideal. For instance, in Iowa, 40 percent of the residents live in rural communities. These communities often see health disparities, particularly with hypertension, diabetes and high cholesterol. Drake University has partnered with Certintell and Tabula Rasa to provide remote monitoring services for rural Iowa communities, along with the assistance of health coaches and medication risk assessments to drive behavior change. Many health systems continue to launch similar projects this year.
To launch your own, reach out to us!
Maximizing RTM & CTBS
Remote Therapeutic Monitoring, RTM, is the newest CMS-introduced spinoff of RPM. It includes the monitoring of non-physiologic data, such as musculoskeletal and respiratory systems, therapy adherence or therapy response. For obvious reasons, this extends the practice of RPM to a wider range of providers. But what is important to note is that this new service wasn’t introduced by way of innovation, but rather by a new government policy. This means in 2022, more system-level changes could occur to make remote monitoring a widespread and standard practice in the health care industry.
It’s likely that 2022 will be a big year of discovery in the remote monitoring sector, especially as the industry navigates the advantages and complications of RTM. Clinicians who choose to implement the service will likely aim to increase patient utilization and decrease hospitalizations. However, these care teams will likely need some help in doing so. This year, we could see more diverse cross-sector partnerships as the industry works together to reimagine care for patients under this newest service.
RTM is actually a service under Communication-Technology Based Services, an umbrella category for a range of virtual health services. Crafted by CMS, CTBS is composed of RTM, virtual check-ins, e-visits, remote evaluations of images, and audio-only patient visits. Generally, the services under CTBS are more accessible and more affordable forms of mHealth. In 2022, CMS finalized some favorable flexibilities for FQHCs in its Physician Fee Schedule, including continued audio-only reimbursements. Given its benefits, CTBS may soon become not only an easily reimbursable group of services, but mainstream in the care environment.
How Certintell Can Help
Certintell is a leader in remote monitoring for underserved populations. Whether you’re looking to get on trend, or innovate your existing remote monitoring services, we can work with your team to develop perfectly tailored programs. Whether your organization is a payer or provider, Certintell has innovative solutions for everyone.
SOURCES
² https://www.healthcareitnews.com/news/rpm-will-be-new-standard-care-new-study-say
³ https://letstalkinteractive.com/blog/top-ten-medicare-remote-patient-monitoring-faqs
⁴ https://www.investors.com/news/technology/digital-health-firms-advance-wearable-tech-at-ces-2022/